Showing posts with label addiction treatment. Show all posts
Showing posts with label addiction treatment. Show all posts
Monday, June 20, 2016
Addiction Treatment Industry at the Crossroads
How unethical treatment shills hunt down patients.
Check this account at Huffington Post by Ryan Grim: "Addiction Treatment Industry Worried Lax Ethics Could Spell Its Doom."
Eye-opening.
Check this account at Huffington Post by Ryan Grim: "Addiction Treatment Industry Worried Lax Ethics Could Spell Its Doom."
Eye-opening.
Labels:
addiction treatment,
inside rehab,
rehab
Monday, February 17, 2014
Acamprosate For Alcohol: Why the Research Might Be Wrong
“Occasionally,” reads the opening sentence of a commentary published online last month in Neuropsychopharmacology, “a paper comes along that fundamentally challenges what we thought we knew about a drug mechanism.” The drug in question is acamprosate, and the mechanism of action under scrutiny is the drug’s ability to promote abstinence in alcoholics. The author of the unusual commentary is Markus Heilig, Chief of the Laboratory of Clinical and Translational Studies at the National Institute on Alcohol Abuse and Alcoholism (NIAAA).
Acamprosate, in use worldwide and currently the most widely prescribed medication for alcohol dependence in the U.S., may work by an entirely different mechanism than scientists have believed on the basis of hundreds of studies over decades. Rainer Spanagel of the Institute of Psychopharmacology at the University of Heidelberg, Germany, led a large research group in revisiting research that he and others had performed on acamprosate ten years earlier. In their article for Neuropsychopharmacology, Spanagel and coworkers concluded that a sodium salt version of acamprosate was totally ineffective in animal models of alcohol-preferring rats.
“Surprisingly,” they write, “calcium salts produce acamprosate-like effects in three animal models…. We conclude that N-acetylhomotaurinate is a biologically inactive molecule and that the effects of acamprosate described in more than 450 published original investigations and clinical trials and 1.5 million treated patients can possibly be attributed to calcium.”
At present, the Food and Drug Administration (FDA] has approved three drugs for alcoholism— Antabuse, naltrexone, plus acamprosate in 2004. In addition, there is considerable clinical evidence behind the use of four other drugs—topiramate, baclofen, ondansetron, and varenicline. Acamprosate as marketed is the calcium salt of N-acetyl-homotaurinate, a close relative of the amino acid taurine. It has also been found effective in European studies.
What did scientists think acamprosate was doing? Various lines of research had linked acamprosate to glutamate transmission. Changes in glutamate transmission have been directly implicated in active alcoholism. A decade ago, the Spanagel group had decided that acamprosate normalized overactive glutamate systems, and hypothesized that acamprosate was modulating GABA transmission. So it became known as a “functional glutamate antagonist.” But specific mechanisms have remained elusive ever since.
Now, as Heilig comments, “the reason it has been difficult to pin down the molecular site of acamprosate action may simply be because it does not exist. Instead, the authors propose that the activity attributed to acamprosate has all along reflected actions of the Ca++ it carries.” As the researcher paper explains it: “N-acetylhomotaurinate by itself is not an active psychotropic molecule…. We have to conclude that the proposed glutamate receptor interactions of acamprosate cannot sufficiently explain the anti-relapse action of this drug.” Further work shows that acamprosate doesn’t interact with glutamate binding sites at all. In other words, calcium appears to be the major active ingredient in acamprosate. Animal studies using calcium chloride or calcium gluconate reduced alcohol intake in animals at rates similar to those seen in acamprosate, the researchers claim.
Subsequently, the researchers revisited the earlier clinical studies, subjected them to secondary analysis, and concluded that “in acamprosate-treated patients positive outcomes are strongly correlated with plasma Ca++ levels. No such correlation exists in placebo-treated patients.” In addition, calcium salts delivered via different carrier drugs replicated the suppression of drinking in the earlier animal findings.
Where there cues pointing toward calcium? The researchers conclude that “calcium sensitivity of the synapse is important for alcohol tolerance development, calcium given intraventricularly significantly enhances alcohol intoxication in a dose-dependent manner,” and “activity of calcium-dependent ion channels modulate alcohol drinking.”
Interestingly, in the late 50s and early 60s, there was a brief period of interest in calcium therapy for the treatment of alcoholism. In 1964, the Journal of Psychology ran an article titled “Intensive Calcium Therapy as an Initial Approach to the Psychotherapeutic Relationship in the Rehabilitation of the Compulsive Drinker.” Now it appears possible that a daily dose of acamprosate is effective for some abstinent alcoholics because it raises calcium plasma levels. Calcium supplements may be in for a round of intensive clinical testing if these findings hold up.
The authors now call for “ambitious randomized controlled clinical trials,” to directly compare “other means of the Ca++ delivery as an approach to treat alcohol addiction. Data in support of a therapeutic role of calcium would open fascinating clinical possibilities.” Indeed it would.
Spanagel R., Vengeliene V., Jandeleit B., Fischer W.N., Grindstaff K., Zhang X., Gallop M.A., Krstew E.V., Lawrence A.J. & Kiefer F. (2013). Acamprosate Produces Its Anti-Relapse Effects Via Calcium, Neuropsychopharmacology, 39 (4) 783-791. DOI: 10.1038/npp.2013.264
Monday, February 3, 2014
The Anthropology of Addiction
Can we ever integrate neuroscience and social science?
Bielefeld, Germany—
The last in a series of posts about a recent conference, Neuroplasticity in Substance Addiction and Recovery: From Genes to Culture and Back Again. The conference, held at the Center for Interdisciplinary Research (ZiF) at Bielefeld University, drew neuroscientists, historians, psychologists, philosophers, and even a freelance science journalist or two, coming in from Germany, the U.S., The Netherlands, the UK, Finland, France, Italy, Australia, and elsewhere. The organizing idea was to focus on how changes in the brain impact addiction and recovery, and what that says about the interaction of genes and culture. The conference co-organizers were Jason Clark and Saskia Nagel of the Institute of Cognitive Science at the University of Osnabrück, Germany. Part One is here. Part Two is here. Part Three is here.
The disciplines of psychiatry and neurology are being brought intellectually closer to each other. One can foresee the day in the not-too-distance future when resident physicians in both disciplines will share a common year of training, comparable to the year of residency training in internal medicine for physicians who go on to specialize in widely different areas.
— Eric Kandel, In Search of Memory
Anthropology is arguably a perfect discipline within which to connect the two often-conflicting facets of addiction—its fundamental neuroarchitecture, and the socioenvironmental influences that shape this basic biological endowment. In The Encultured Brain, published by MIT Press, co-editors Daniel H. Lende and Greg Downey make an articulate call for a merger of interests, in an attempt to combine laboratory research with anthropological fieldwork. The term “neuroanthropology,” meant to denote this combination of anthropology and brain science, was evidently coined by Stephen Jay Gould. A number of thinkers have dipped into this arena over the years, including Melvin Konner, Sarah Hrdy, Norman Cousins, Robert Sapolsky, and Antonio Damasio. The term gained a more solid foothold when Lende and Downey began their Neuroanthropology blog, now at PLOS blogs.
The term has the advantage of meaning exactly what it says: an integrative approach to the complicated matter of how our genetic endowment is influenced by our cultural endowment. Or vice versa, if you prefer. Here, from the introductory chapter, is the short definition of neuroanthropology: “Forms of enculturation, social norms, training regimens, ritual, language, and patterns of experience shape how our brains work and are structured…. Without material change in the brain, learning, memory, maturation, and even trauma could not happen…. Through systematic change in the nervous system, the human body learns to orchestrate itself. Cultural concepts and meanings become neurological anatomy.” From the point of view of actual study, there is no choice but to join these two when possible—a task make more difficult by the rampant “biophilia” found among anthropologists and sociologists, as well as the countering notion among biologists that anthropology does not make the cut as a “real” science.
Co-author Daniel Lende, an associate professor in the Department of Anthropology at the University of South Florida, was one of the presenters at the Bielenfeld conference. Lende did his Ph.D. work on adolescent substance abuse in Bogota, Colombia, and told the group that years of research “showed me that addiction is profoundly neuranthropological.” Lende told the audience that the “combination of neuroscience and ethnography revealed that addiction is a problem of involvement, not just of pleasure or of self.”
This approach calls for applying a critical eye to strictly brain-based explanations that ignore both environmental influence and biochemical individuality. And it opens up the possibility that anthropologists may be incorporating neuroimaging technology into their working tool kit. While the neuroanthropology movement has been mostly a product of the anthropology side thus far, Lende said. But increasingly, cognitive scientists are joining in.
“As neuroanthropologists, we’re not trying to solve problems in the lab or in the clinic, but rather to take the results of that sort of work, and look at what’s happening to those brains in the wild,” Lende said.
Repeated patterning comes from social environments, he said. “We have to deal with how cultural practices and developmental experiences can shape and mold the brain, and how that has an effect on the production of human variation, not just sets of beliefs you can take on and put off.” The cultural practice of skull shaping, for example, is “impossible to understand without taking into account both the cultural practices that drive it, and the early plasticity in bone formation that allows it biologically.”
Culture, said Dr. Lende, “can bring different elements into one package. It doesn’t have to be the biology side that does all the work. You can take the cultural strands and knit them into something really unusual that you wouldn’t necessarily see in the world. With cultural tools, we are using are brain in ways not necessarily built into it from the start.”
But attending to all of this requires thinking of neural plasticity in novel ways, Lende said. “Hardwiring isn’t quite as hard as we once thought. The lifespan of these circuits set early in life isn’t what we thought.” The brain can use sensory input in ways we don’t yet understand. Lende pointed to “significant recovery from stroke, which was not viewed as possible a couple of decades ago.”
“You have to be critical both of the neuroscience and some of its limitations, and also the anthropologists, who are sometimes saying, ‘it’s got to be all sociocultural.’ That’s not always a good explanation for something as complex as addiction.”
Lende believes that anthropology needs to pursue the impact of “biological embedding, or how experiences get under the skin” to alter human biological and developmental processes. “You can have differential vulnerabilities to biological embedding, coupled with differential environmental vulnerability.”
Dr. Lende points to the well documented clinical finding that exercise enhances neuroplasticity. “And exercising has been shown in various labs to reduce craving,” he said. “What’s important from my community-based orientation is, what sort of interventions or strategies can we have that are low cost and be used in non-professional settings. Can we motivate people to do it? What are the barriers?”
Subjective experience is hard to get at, but that’s a problem anthropologists think about all the time. “I asked the kids in Columbia, if your drug use were a place, Lende said, “ then what sort of place would that be? Kids who’d never tried drugs didn’t get the question, but a kid with heavy cigarette use who had just quit, and who had recovered recently from using too much cocaine and crack, looked at his fingers, referring to cigarettes, and said, ‘a world in there? No. But with cocaine, yes.”
Tuesday, January 28, 2014
Going Deep: Surgery For Addiction?
Controversial DBS technique shows early promise for Parkinson’s, Tourette’s.
Bielefeld, Germany—
The third in an irregular series of posts
about a recent conference, Neuroplasticity in Substance Addiction and Recovery: From Genes to
Culture and Back Again. The conference, held at the Center for
Interdisciplinary Research (ZiF) at Bielefeld University, drew
neuroscientists, historians, psychologists, philosophers, and even a freelance
science journalist or two, coming in from Germany, the U.S., The Netherlands,
the UK, Finland, France, Italy, Australia, and elsewhere. The organizing idea
was to focus on how changes in the brain impact addiction and recovery, and
what that says about the interaction of genes and culture. The conference
co-organizers were Jason Clark and Saskia Nagel of the Institute of Cognitive Science at the University of Osnabrück,
Germany. Part One is here.
Part Two is here.
All addictive drugs increase the production of dopamine in the nucleus accumbens, as do other highly pleasurable activities. Part of the medial forebrain bundle (MFB), which mediates punishment and reward, the nucleus accumbens is the ultimate target for the dopamine released by the ingestion of cocaine, for example. The nucleus accumbens is a very old and evolutionarily well-preserved structure in the brain. If you remove large slices of the nucleus accumbens, or knock it out entirely, animals no longer want addictive drugs.
This is essentially the same pathway that regulates our food and water-seeking behavior. By directly or indirectly influencing the molecules of pleasure, alcohol and other drugs trigger key neurochemical events that are central to our feelings of both reward and disappointment. In this sense, the reward pathway is a route to both pleasure and pain. Studies of the nucleus accumbens have demonstrated abnormal firing rates in scanned addicts who were deep into episodes of craving. The craving for a reward denied causes dopamine levels in the nucleus accumbens to crash dramatically, as they do when users go off drugs.
During his presentation in Bielefeld, “Stimulating the Addictive Brain,” Dr. Jens Kuhn of the University Hospital of Cologne walked the audience through an explanation of one of the most controversial addiction treatment options of all, known as deep brain stimulation. For those unfamiliar with DBS, this surgical procedure uses implanted brain electrodes and a subdermal set of wires connected to a small power source to directly stimulate a designated area of the brain via electric current. Deep brain stimulation (DBS) is becoming an established treatment option for some movement disorders, in particular Parkinson’s disease. It is also being investigated for obsessive–compulsive disorder, major depression, and Tourette’s syndrome.
Kuhn and his researchers, the first German group to investigate deep brain stimulation beginning in 2002, started by investigating Tourette’s and OCD. But soon, Kuhn said, it became clear that “valid animal studies show significant induced improvement in cocaine, morphine and alcohol addiction behavior following DBS of the nucleus accumbens…. the few patients who underwent DBS surgery for addiction remained abstinent or had a major reduction of relapses.”
This is essentially the same pathway that regulates our food and water-seeking behavior. By directly or indirectly influencing the molecules of pleasure, alcohol and other drugs trigger key neurochemical events that are central to our feelings of both reward and disappointment. In this sense, the reward pathway is a route to both pleasure and pain. Studies of the nucleus accumbens have demonstrated abnormal firing rates in scanned addicts who were deep into episodes of craving. The craving for a reward denied causes dopamine levels in the nucleus accumbens to crash dramatically, as they do when users go off drugs.
During his presentation in Bielefeld, “Stimulating the Addictive Brain,” Dr. Jens Kuhn of the University Hospital of Cologne walked the audience through an explanation of one of the most controversial addiction treatment options of all, known as deep brain stimulation. For those unfamiliar with DBS, this surgical procedure uses implanted brain electrodes and a subdermal set of wires connected to a small power source to directly stimulate a designated area of the brain via electric current. Deep brain stimulation (DBS) is becoming an established treatment option for some movement disorders, in particular Parkinson’s disease. It is also being investigated for obsessive–compulsive disorder, major depression, and Tourette’s syndrome.
Kuhn and his researchers, the first German group to investigate deep brain stimulation beginning in 2002, started by investigating Tourette’s and OCD. But soon, Kuhn said, it became clear that “valid animal studies show significant induced improvement in cocaine, morphine and alcohol addiction behavior following DBS of the nucleus accumbens…. the few patients who underwent DBS surgery for addiction remained abstinent or had a major reduction of relapses.”
Carrie Wade and others at the Scripps Research Institute and Aix-Marseille University in France electrically stimulated the subthalamic nucleus and got addicted rats to take less heroin and become less motivated for the task of bar pressing to receive the drug. Earlier work had demonstrated a similar effect in rats’ motivation for cocaine use. “This research takes a non-drug therapy that is already approved for human use and demonstrates that it may be an option for treating heroin abuse,” Wade said in a prepared statement.
Dr. Kuhn told the audience that DBS is a “focused neuromodulation procedure to enrich electrical activity” applied to certain brain regions and requiring only “minimally invasive” surgery. In the case of DBS surgery for addiction, which Dr. Kuhn has performed in clinical settings, the target is the nucleus accumbens, which Kuhn called “the key player in the so-called limbic reward loop.”
The problem is that these investigations, while positive in many cases, are small and scattered thus far, and do not represent a systematic investigation of the procedure by the field of neuroscience at large. Not yet, anyway. And maybe not ever. There are very few published studies on human addicts, Kuhn said, “but luckily, the ethical implications of DBS are being more and more discussed.”
Unfortunately, as Kuhn pointed out, “neurosurgical interventions in psychiatric patients raise ethical considerations not only based on the disreputable experiences of the era of psychosurgery.” But that’s a good starting point. The procedure, despite one’s best efforts, conjures up images of “psychosurgery”—prefrontal lobotomies, or early electroconvulsive shock therapy (ECT). It doesn’t help that the likeliest mechanism of action that explains DBS is that high frequency stimulation causes functional lesions at the specific brain sites. From almost every angle, it seems ham-handed and crude—until you see some videos of results, like this one of a Tourette’s patient: Video
Kuhn acknowledged that a number of medical professional believe DBS is a poor choice for addiction, and its use “is premature due to expenses, possible risks and the assumed poor scientific rationale of the method in this field.” In a letter to the journal Addiction, Adrian Carter and Wayne Hall of the University of Queensland, Australia, noted that some of the positive reports come from China, where scientists have experimented with ablation of portions of the nucleus accumbens and other brain areas. And it seems to work. So, one cure for addiction has been discovered already—but surgically removing chunks of the midbrain isn’t likely to catch on, except as a seminar topic for medical ethicists. Carter and Hall call the evidence base for the safety and efficacy of DBS in addiction “weak,” and argue that “the addition of an expensive neurosurgical treatment that costs of the order of $50,000 will worsen this situation by utilizing scare health resources to treat a very small number of patients with the income to pay for it.”
In a history of “stereotactic lesions” as a treatment for movement disorders, researchers at The George Washington University School of Medicine and Health Sciences reviewed efforts to expand the use of DBS to include specific psychiatric disorders like depression and obsessive-compulsive disorders. Writing in the Journal of Neurosurgery in 2010, they concluded that “addiction and schizophrenia showed the least improvement from surgery. Therefore, pursuing the treatment of these disorders with DBS using the targets in these studies may be ineffective.”
The Neurotech Business Report recently documented that St. Jude Medical, a manufacturer of surgical devices, has shut down its clinical trial of DBS for depression (h/t Vaughan Bell). The company’s website said “The BROADEN (BROdmann Area 25 DEep brain Neuromodulation) Study” has been closed and is no longer enrolling participants. The article suggests that “the complexity of specifying the precise brain circuits involved with major depression” may have been the reason for halting the trial.
Known risks associated with deep brain stimulation placement include: dizziness, infection, loss of balance, and speech or vision problems. In addition, the devices, wires and leads that make up the system, which are all implanted in the brain or under the skin, can break or fail in various ways. DBS can also alter glucose metabolism and food intake in lab rats. Altogether, there are few case reports, and the mechanism of action remains essentially uncharacterized. In the case of addiction, this is one treatment that does not seem ready for prime time. It would be premature to move DBS beyond the clinical trial stage in humans without additional data.
Wednesday, January 22, 2014
Drug Craving, or How to Be Your Own Worst Enemy
Plus the disease model, warts and all.
Bielefeld, Germany—
The second in an irregular series of posts about a recent conference, Neuroplasticity in Substance Addiction and Recovery: From Genes to Culture and Back Again. The conference, held at the Center for Interdisciplinary Research (ZiF) at Bielefeld University, drew neuroscientists, historians, psychologists, philosophers, and even a freelance science journalist or two, coming in from Germany, the U.S., The Netherlands, the UK, Finland, France, Italy, Australia, and elsewhere. The organizing idea was to focus on how changes in the brain impact addiction and recovery, and what that says about the interaction of genes and culture. The conference co-organizers were Jason Clark and Saskia Nagel of the Institute of Cognitive Science at the University of Osnabrück, Germany. Part One is here.
Marc Lewis, a developmental neuroscientist who is currently professor of human development and applied psychology at Radboud University in The Netherlands, and who spent five days discussing addiction with the Dalai Lama and a small group of scientists, scholars, and addiction specialists in Dharamsala, India, last year, was a late but welcome addition to the speaker list at the conference.
Author of Memoirs of an Addicted Brain, and a self-confessed “drug addict turned neuroscientist,” Dr. Lewis always brings a thought-provoking dual perspective to his work on addiction. (See my review of his book here.) He also blogs here.
In Bielefeld, Dr. Lewis offered up a wide-ranging view of what addiction is and is not, linking neuroscience, psychology, and Buddhism in the process.
Craving is “the one condition all addicts agree is their worst enemy,” Lewis said. “This is one place where science and subjectivity have to come together. Scientists need to focus on this, because addicts are completely unanimous about it. This is the enemy. It’s not physical withdrawal symptoms, it’s not relief. It is craving.”
Buddhism teaches that “craving is the fundamental engine of personality development,” Lewis said. “It’s what keeps us going around and around.” But if you don’t much like the notion of the wheel of reincarnation, Lewis suggested, then you can contemplate “the cyclical nature of how we repeat patterns in life that lead to suffering.”
“Craving is such an unpleasant state, that after a while, you end up doing it, you get the drugs. I did opiates, and I would spend hours and hours trying to sit on my hands, trying to watch something on TV, trying to go for a walk, and finally, there’s this thing that keeps rising in the background, and it doesn’t go away. It was a constantly growing tension, an anxiety and discomfort, that came from very deep down. You spend most of your energy trying to hold this thing at bay, and according to the ego depletion literature, you can’t do that for very long. These cognitive control centers just give up. They are limited resources.”
Craving is not a steady state. It grows. “Neuroscience helps us understanding why craving is so nasty.” Enter “delay discounting,” a term from behavioral economics used by several speakers during the conference. Delay discounting is the proposition that the perceived value of something rises steeply as the reward gets closer in time. A variation of this idea is seen in the classic marshmallow test for children: One marshmallow now, or two if you wait until later?
“Craving traps you in delay discounting,” said Lewis. “Immediate reward is worth more than imagined future happiness. The job of dopamine in the striatum is to increase the attractiveness or value of one goal, and to reduce the attractiveness and value of all the other goals. This is a brain that is well designed for addiction. You get tons of dopamine rising up in anticipation of reward. So you’re really stuck in the immediate. At which point you’ve effectively lost contact with the rest of your life. In the narrative of who you are, you can’t even include next week, or the next morning.”
Nonetheless, Lewis finds serious problems with the standard disease model of addiction, as championed by NIDA’s Nora Volkow and other in the NIH, however brain-based he may be. As a developmental neuroscientist, Lewis is predisposed to viewing the brain as a locus of change by definition. “The disease model uses brain change as a foundational premise. But brains change with development, anyway. And in fact, brains are designed to change.”
Any proper model of addiction, he insisted, has to correspond with what we know about brain change. “But it also has to correspond with addicts’ experiences. I was a drug addict from about age 25 to 30. I was in really bad shape. And now I talk with a lot of drug addicts, and one of the things that I keep hearing is that scientists and clinicians don’t really know what they’re doing—they don’t know where to go with it. They know that addiction is really nasty, but they don’t know what it’s like, unless they’ve been there.”
Lewis offered a view of addiction that shifts the semantic focus from disease to development. The drug is not the culprit. By reconceptualizing addiction as a developmental disorder, he suggested, we can move the debate forward into the world, where the action is:
Addiction results from accelerated learning, the acquisition of thought patterns that rapidly self-perpetuate because of the brain’s tendency to become sensitized to highly attractive rewards. This is a developmental process, accelerated by a neurochemical feedback loop that is particular to strong attractions. Like other developmental outcomes, addiction isn’t easy to reverse, because it’s based on synaptic restructuring. Like other developmental outcomes, it arises from neural plasticity, and uses it up at the same time.
And the mechanisms responsible are the same ones responsible for many things that involve desire, learning, reward seeking, and compulsive behavior—including the so-called behavioral addictions like overeating and compulsive sex. However, “the severe consequences of addiction don’t make it a disease, any more than the consequences of violence make violence a disease.”
In an email exchange after the conference, I followed up with Dr. Lewis on some of these matters, and he sent me the following additional thoughts on the “diseasing” of addiction:
Proponents of the disease model argue that addiction changes the brain. And they're right: it does. But the brain changes anyway, at every level, from gene expression, to cell density, to the size and shape of the cortex itself. Of course, neuroscientists who subscribe to the disease model must know that brains change over development. Their take on pathological brain change would have to be very specific in order to be convincing. For example, they would have to show that the kind (or extent or location) of brain change characteristic of addiction is nothing like that observed in normal learning and development. But this they cannot do. The kind of brain changes seen in addiction also show up when people take up rock collecting, fall in love, learn how to cook, or become obsessed with their appearance. The brain contains only a few major traffic routes for learning and goal seeking. And, like the main streets of a busy city, they are often under construction. Brain disease may be a useful metaphor for how addiction seems, but it's not a valid explanation for how it actually works.
Wednesday, December 18, 2013
What Mark Kleiman Wants You To Know About Drugs
The public policy guru guiding state legalization efforts.
Mark A. R. Kleiman is the Professor of Public Policy at UCLA, editor of the Journal of Drug Policy Analysis, author of many books, and generally regarded as one of the nation’s premier voices on drug policy and criminal justice issues. Mr. Kleiman provides advice to local, state, and national governments on crime control and drug policy. When the state of Washington needed an adviser on the many policy questions they left unanswered with the passage of I-502, which legalized marijuana in that state, they turned to Kleiman.
In the past two years, Kleiman has co-authored to Q and A-style books: Drugs and Drug Policy: What Everyone Needs to Know (2011) with Jonathan P. Caulkins and Angela Hawken; and Marijuana Legalization: What Everyone Needs to Know (2012) with Hawken, Caulkins, and Beau Kilmer.
Here, excerpted from the two books, is a brief sampling of Kleiman and his colleagues on a variety of drug and alcohol issues.
Is marijuana really the nation’s leading cash crop?
“Alas, the facts say otherwise. Analyses purporting to support the claim must contort the numbers, citing the retail price of marijuana but the farmgate price of other products, or pretending that all marijuana consumed in the United States is sinsemilla, or ignoring the fact that most marijuana used in the United States is imported, or simply starting with implausible estimates of U.S. production…. marijuana [is] in the top fifteen, but not the top five, cash crops, ranking somewhere between almonds and hay, and perhaps closest to potatoes and grapes.”
How much drug-related crime, violence, and corruption would marijuana legalization eliminate?
“Not much…. Eighty-nine percent of survey respondents report obtaining marijuana most recently from a friend or relative, and more than half (58 percent) say the obtained it for free. That stands in marked contrast to low-level distribution of heroin and crack which often occurs in violent, place-based markets controlled by armed gangs.”
How much would legal marijuana cost to produce?
“The punch line is that full legalization at the national level—as opposed to only legalizing possession and retail sale—could cut production costs to just 1 percent of current wholesale prices…. This would make legal marijuana far and away the cheapest intoxicant on a per-hour basis.”
How would legalization affect me if I’m a marijuana grower?
“It would almost certainly put you out of business. At first glance, legalization might seem like a great opportunity for you…. But legalization will completely upend your industry, and the skills that made you successful at cultivating illegal crops will not have much value. A few dozen professional farmers could produce enough marijuana to meet U.S. consumption at prices small-scale producers couldn’t possibly match. Hand cultivators would be relegated to niche markets for organic or specialty strains.”
Would marijuana regulations and taxes in practice approach the public health ideal?
“If there is a licit, for-profit marijuana industry, one should expect its product design, pricing, and marketing actions to be designed to promote as much frequent use and addiction as possible. Efforts to tax and regulate in ways that promote public health would have to contend with an industry mobilizing its employees, shareholders, and consumers against any effective restriction. Since the industry profits from problem users, we should expect that lobbying effort to be devoted to blocking policies that would effectively control addiction. The alcohol and tobacco industries provide good examples.”
Can we persuade children not to use drugs?
"Even the best prevention programs have only modest effects on actual behavior, and may programs have no effect at all on drug use…. Anesthesiologists know far more about drugs and drug abuse than could possibly be taught in middle-school prevention programs; nonetheless, they have high rates of substance abuse, in part because they have such easy access.”
Why is there a shortage of drug treatment?
“Some specific categories—especially those in need of residential care, and more especially mothers with children in need of residential care—face chronic shortages. But if we had enough capacity for all those who need treatment, many of those slots would be empty because not all the people who ought to fill them want treatment.”
How much money is involved?
“Most of the numbers about drug abuse and drug trafficking that officials peddle to credulous journalists are little better than fiction. Estimates of hundreds of billions of dollars per year in international drug trade—which would make it comparable to food, oil, and arms—do not have a basis in the real world. The most recent serious estimate of the total retail illicit drug market in the United States—by all accounts the country whose residents spend the most on illicit drugs—puts the figure at about $65 billion.”
When it comes to drugs, why can’t we think calmly and play nice?
“American political analysts talk about ‘wine-track (college-educated) and ‘beer track’ (working-class) voters…. So the politics of drug policy is never very far from identity politics…. The notion that illicit drug taking is largely responsible for the plight of minorities (and of poor people generally) and that income-support programs have the perverse consequence of maintaining drug habits has been a staple of a certain form of American political rhetoric at least since Ronald Reagan.”
Are we stuck with our current alcohol problem?
"By no means…. tripling the tax would raise the price of a drink by 20 percent and reduce the volume of drinking in about the same proportion. Most of the reduced drinking would come from heavy drinkers, both because they dominate the market in volume terms and because their consumption is more price-sensitive…."
Sunday, September 22, 2013
Do Addicts Benefit From Chronic Care Management?
Controversial JAMA study questions orthodox addiction treatment.
What is the best way to treat addiction? The conventional wisdom has been to treat it with chronic care management (CCM), the same approach used for various medical and mental illnesses. But a study in the Journal of the American Medical Association (JAMA) purports to demonstrate that “persons with alcohol and other drug dependence who received chronic care management (CCM)” were no more likely to become abstinent that those who received nothing beyond a timely appointment with a primary care physician, and a list of addiction treatment resources.
563 patients were divided into a chronic care management group and a primary care group. The chronic care management group received extended care under a primary care physician, plus
“motivational enhancement therapy; relapse prevention counseling; and on-site medical, addiction, and psychiatric treatment, social work assistance, and referrals (to specialty addiction treatment mutual help.)” The primary care group got the aforementioned doctor’s appointment and printed list of treatment resources.
The study by researchers at Boston Medical Center found that “there was no significant difference in abstinence from opioids, stimulants, or heavy drinking between the CCM (44%) and control (42%) groups. No significant differences were found for secondary outcomes of addiction severity, health-related quality of life, or drug problems.”
But there are limitations. To wit:
1) Small sample size. 282 patients in a Boston Hospital’s chronic care management facility, and 281 participants farmed out to a primary care physician, is the total. Given the known failure rates for chronic care management as applied to smoking, diabetes, and mental illness, and variability in the counseling given the control group by individual physicians, 563 people isn’t really a sufficient cohort to be anything but suggestive. And, since many alcoholics and other drug addicts get sober by means of their own efforts, independent of formal medical intervention, percentage comparisons of such small groups are problematic in addiction studies.
2) Hard Core Cases Only. “Most study participants were dependent on both alcohol and other drugs, recruited from a detoxification unit, had substantial mental health symptoms had recently been homeless, and were not necessarily seeking addiction treatment,” according to the JAMA study. Okay, who might the findings not apply to? “Addiction treatment-seeking or less severely affected populations or to populations recruited elsewhere.”
3) Mostly self-reported data. The investigators assessed main outcomes by self-report. “Biological tests are inadequate for detecting substance use, particularly when it is not recent,” they explain. “Substance use problems and health-related quality of life are best assessed by self-report.” Outcomes were also based on self-reported 30-day abstinence.
4) Alcohol abusers did better under CCM. The research documented “a small effect on alcohol problems among those with dependence.” On alcoholics, in other words. “No subgroup effects were found except among those with alcohol dependence, in whom CCM was associated with fewer alcohol problems.” So CCM works, at least to a degree, for alcoholics, even in this study. Nonetheless, the study concludes: “CCM for substance dependence in primary care is not effective, at least not as implemented in this study and population.” (Note the caveats, and see #2 above)
5) Treatment fails for many reasons. One reason might be that the length of treatment was too short. According to the study, the intervention group “had, on average, 6 CCM visits….” Moreover, “the whole group improved over time; the change most likely was due to many participants having been enrolled at a detoxification unit….” The researchers also admit that “assessment effects in treatment trials are inconsistent and poorly understood and often absent in studies of people not seeking treatment.”
It may even be true that chronic care management, which seems so logical and successful an approach for everything from depression to smoking cessation, doesn’t work any better for drug addiction than a simple doctor’s visit and a handful of pamphlets. But this study doesn't clinch the case.
Graphics Credit: http://www.ihi.org
Saitz R. (2013). Chronic Care Management for Dependence on Alcohol and Other Drugs: The AHEAD Randomized Trial
Monday, April 22, 2013
Let the Light Shine In: Addiction and Optogenetics
Study says laser light can turn cocaine addiction on and off in rats.
Francis Collins, the director of the National Institutes of Health (NIH), had one word for it: “Wow.”
Writing in the director’s blog at the online NIH site, Collins said that a team of researchers from NIH and UC San Francisco had succeeded in delivering “harmless pulses of laser light to the brains of cocaine-addicted rats, blocking their desire for the narcotic.”
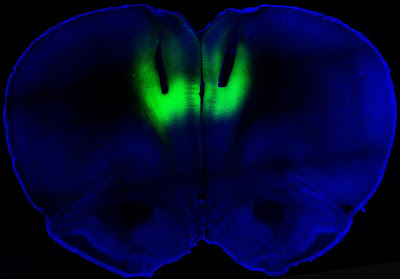
Wow, indeed. It didn’t take long for the science fiction technology of optogenetics to make itself felt in addiction studies. The idea of using targeted laser light to strengthen or weaken signals along neural pathways has proven surprisingly robust. The study by the NIH and the University of California at San Francisco, published in Nature, showed that lab rats engineered to carry light-activated neurons in the prefrontal cortex could be deterred from seeking cocaine. Conversely, laser light used in a way that reduced signaling in this part of the brain led previously sober rats to develop a taste for the drug. As Collins described the work:
The researchers studied rats that were chronically addicted to cocaine. Their need for the drug was so strong that they would ignore electric shocks in order to get a hit. But when those same rats received the laser light pulses, the light activated the prelimbic cortex, causing electrical activity in that brain region to surge. Remarkably, the rat’s fear of the foot shock reappeared, and assisted in deterring cocaine seeking.
All this light zapping took place in a brain region known as the prelimbic cortex. In their paper, Billy T. Chen and coworkers said that they “targeted deep-layer pyramidal prelimbic cortex neurons because they project to brain structures implicated in drug-seeking behavior, including the nucleus accumbens, dorsal striatum and amygdala.” These three subcortical regions are rich in dopamine receptors. In rats that had been challenged with foot shocks before being offered cocaine, “optogenetic prelimbic cortex stimulation significantly prevented compulsive cocaine seeking, whereas optogenetic prelimbic cortex inhibition significantly increased compulsive cocaine seeking.”
What this demonstrates is that similar regions in the human prefrontal cortex, known to regulate such actions as decision-making and inhibitory response control, may be “compromised” in addicted people. This abnormally diminished excitability in turn “impairs inhibitory control over compulsive drug seeking…. We speculate that crossing a critical threshold of prelimbic cortex hypoactivity promotes compulsive behaviors”
This all sounds vaguely unsettling; sort of a cross between phrenology and lobotomy. But it is no such thing, and the study authors believe that stimulation of the prelimbic cortex “might be clinically efficacious against compulsive seeking, with few side effects on non-compulsive reward-related behaviors in addicts.” For now, the researchers confess that they don’t know whether the reduction in cocaine seeking is caused by altered emotional conditioning, or pure cognitive processing.
Actually, nobody expects optogenetics to be used in this way with humans. The thinking is that transcranial magnetic stimulation, the controversial technique that employs noninvasive electromagnetic stimulation at various points on the scalp to alter brain behavior, would be used in place of invasive zaps with lasers. Expect to hear about clinical trials to test this theory in the near future. David Shurtleff, acting deputy director at the National Institute on Drug Abuse (NIDA), said in a prepared statement that the research “advances our understanding of how the recruitment, activation and the interaction among brain circuits can either restrain or increase motivation to take drugs.”
Chen B.T., Yau H.J., Hatch C., Kusumoto-Yoshida I., Cho S.L., Hopf F.W. & Bonci A. (2013). Rescuing cocaine-induced prefrontal cortex hypoactivity prevents compulsive cocaine seeking, Nature, 496 (7445) 359-362. DOI: 10.1038/nature12024
Photo credit: Billy Chen and Antonello Bonci
Sunday, March 24, 2013
More Hard Facts About Addiction Treatment
“Yes, we take your insurance.”
Recent reportage, such as Anne Fletcher’s book, Inside Rehab, has documented the mediocre application of vague and questionable procedures in many of the nation’s addiction rehab centers. You would not think the addiction treatment industry had much polish left to lose, but now comes a devastating analysis of a treatment industry at “an ethics crossroads,” according to Alison Knopf’s 3-part series in Addiction Professional. Knopf deconstructs the problems inherent in America’s uniquely problematic for-profit treatment industry, and documents a variety of abuses. We are not talking about Medicaid, Medicare, or Block Grants here. Private sector dollars, Knopf reaffirms, do not “guarantee that the treatment is evidence-based, worth the money, and likely to produce a good outcome.” Even Hazelden, it turns out, is prepared to offer you “equine therapy,” otherwise known as horseback riding.
Knopf, who is editor of Alcoholism and Drug Abuse Weekly, was specifically looking at private programs, paid for by insurance companies or by patients themselves. Who is in charge of enforcing specific standards of business practice when it comes to private drug and alcohol rehabs? Does the federal government have some manner of regulatory control? According to a physician with the Substance Abuse and Mental Health Services Administration (SAMHSA), the feds rely on the states to do the regulating. And according to state officials, the states look to the federal agencies for regulatory guidance.
All too often, the states routinely license but do not effectively monitor treatment facilities, or give useful consumer advice. Florida state officials do not even know, with any certainty, exactly how many treatment centers are in operation statewide. And even if state monitoring programs were effective and aggressively applied, “just because something is legal doesn’t mean it’s ethical,” said the SAMHSA official.
“We see this as a pivotal time for the treatment field as we have come to know it,” said Gary Enos, editor of Addiction Professional, in an email exchange with Addiction Inbox. Enos said that “the Affordable Care Act (ACA) will move addiction treatment more into the mainstream of healthcare, and this will mean that treatment centers' referral and insurance practices will come under more scrutiny than ever before.”
Among the questionable practices documented by Knopf:
—Paying bounties and giving gifts to interventionists in return for client referrals.
Under Medicare, paying interventionists for referrals is banned. “In the private sector,” says a California treatment official, “it’s not illegal. But it is unethical.” According to treatment lobbyist Carol McDaid, “kickbacks happen all the time. Treatment centers that are doing this will do so at their own peril in the future,” she told Knopf.
—Giving assurances that treatment will be covered by insurance even though only a portion of the cost is likely to be covered.
Under the Affordable Care Act (ACA), says the SAMHSA official, “We are trying to position people to know more about their benefit package. And the industry has to be more straightforward about what the package will cover.” John Schwarzlose, CEO of the Betty Ford Center, told Knopf that “it’s very hard for ethical treatment providers to compete against insurance bait-and-switch,” when patients are told their insurance is good—but aren’t told that the coverage ends after 7 days, or that the daily maximum payout doesn’t meet the daily facility charges.
—Billing patients directly for proprietary nutrient supplements, brain scans, and other unproven treatment modalities.
“Equine therapy, Jacuzzi therapy, those are nice things, and maybe they help with the process of engagement,” said one therapist. “But people need to recognize that these ancillaries aren’t the essence of getting sober.”
—Engaging in dubious Internet marketing schemes.
You see them on the Internet: dozens and dozens of addiction and rehab referral sites. They list private services in various states, and look, on the surface, like legitimate information resources for people in need. As the owner of a blog about drugs and addiction, I hear from them constantly, asking me for links. “Family members and patients frequently have no way of knowing that a treatment program was really a call center they got to by Googling ‘rehab,’ writes Knopf, “and that the call center gets paid for referring patients to the actual treatment center. They don’t know that a program that promises to ‘work with’ health insurance knows full well the insurance will cover only a few days at the facility, and the rest will have to be paid out of pocket.” She points to a 2011 Wired magazine article, which said the Internet marketing cost of key words like “rehab” and “recovery” can be stratospheric. But “by spending that money—not necessarily providing good service—treatment provides can come out on top on searches. It’s the new marketing to the desperate.”
The group with the most to lose from revelations of this nature is the National Association of Addiction Treatment Providers (NAATP), the association representing both private and non-profit rehab programs. The Betty Ford Center has discontinued its membership in NAATP, a move that reflects the turmoil of the industry today. “It’s crazy that we have treatment centers inviting interventionists and other referents on a cruise, and then giving everyone an iPad,” Schwarzlose said.
As one man who lost his son to an overdose said: “I don’t get it. There’s the American Cancer Society, but I look for drugs and alcohol and I can’t find anything. There’s no National Association for Addictive Disease. How can this be?”
The investigative series will be featured in Addiction Professional’s March/April print issue. Enos believes that “influential treatment leaders are more interested than ever to see this debate aired more publically,” and says that the online publication of Knopf’s articles for the magazine has sparked “a great deal of discussion in treatment centers and on social media, including comments about other questionable practices that harm the field’s reputation.”
Tuesday, February 26, 2013
Addiction Rehab: Everything is Broken
Down the rabbit hole in search of effective treatment.
When I first began researching drugs and addiction years ago, a Seattle doctor told me something memorable. “It’s as if you had cancer,” she said, “and your doctor’s sole method of treatment consisted of putting you in a weekly self-help group.”
I’ve got nothing against weekly self-help groups, to be sure. But as Ivan Oransky, executive editor of Reuters Health and a blogger at Retraction Watch, told me as recently as least year, addiction treatment appeared to be “all selling and self-diagnosis. They’re selling you on the fact that you need to be treated.”
In his introduction to Inside Rehab by Anne M. Fletcher (pictured), treatment specialist and former deputy drug czar A. Thomas McLellan writes that the book is “filled with disturbing accounts of seriously addicted people getting very limited care at exhaustive costs and with uncertain results...”
A common notion about addiction treatment facilities, or rehabs, is they are commonly called, is that they are staffed by professional social workers, certified counselors, and family psychologists, as well as addiction specialists. However: “Of the twenty-one states that specify minimum educational requirements for program or clinical directors of rehabs, only eight require a master’s degree and just six require credentialing as an addiction counselor,” writes Fletcher. Neuroscience journalist Maia Szalavitz, who writes for Time Healthland and specializes in addiction and rehab, told Fletcher that “the addiction field has been about as effectively regulated as banking before the economic crisis in many states.” According to Tom McLellan, counselor and director turnover in addiction treatment programs is “higher than in fast-food restaurants.”
In the United States, where for-profit treatment is prevalent, money does not buy access to superior treatment. Fletcher, author of several self-help books on weight loss and alcoholism, doggedly documents what she learns from visiting treatment facilities and interviewing current and former staff and clients. One difficulty with a book of this kind, based primarily on first-hand accounts, is that the same treatment program can offer vastly contrasting experiences from one client to another. And Fletcher, no fan of the 12 Steps, wants AA and NA to account for themselves in a way those volunteer institutions were never designed to accomplish.
But let’s just say it: Addiction treatment in America is a disaster. Addicts get better despite the treatment industry as often as they get better because of it. How did it all go wrong? Part of the answer is that addiction, like depression, tuberculosis, and other chronic conditions, is a segregated illness, as McLellan explains in his introduction. Traditionally, chronic conditions like alcoholism “were not recognized as medical illnesses, and have only recently been taught in most medical schools and treated by physicians. They were seen as ‘lifestyle problems’ and care was typically provided by concerned, committed individuals or institutions not well connected to mainstream health care.”
For treatment of alcoholism and drug addiction, the work has historically fallen to addicts themselves, due to discrimination, segregation, and stigmatization. This prevailing condition is still seen today in many group treatment programs, which are often administered in large part by former addicts with little or no formal training, rather than medical or psychological professionals. Addiction, as the author’s husband wryly remarked, “is the only disease for which having it makes you an expert.”
Which brings up a central point: Where are all the M.D.s? Doctors aren’t helping, either, when they fail to screen for risky drinking or drug use, or when they automatically refer addicts rather than treating them.
If Christopher Kennedy Lawford’s new book, Recover to Live, is the pretty picture, then Fletcher’s Inside Rehab is the gritty picture, in which most addicts who recover don’t go to treatment, 28 days is not long enough to accomplish anything but detox, group counseling is not always the best way to treat addiction, the 12 Steps are not always essential to recovery, specialty drugs are often needed to treat drug addiction, and, perhaps the most troubling of all, most addiction programs do not offer state-of-the-art approaches to treatment that have been shown to be effective in scientific studies.
What clients get, for the most part, is “group, group, and more group,” Fletcher writes. And in many cases of residential or outpatient rehab, “the clients did most of the therapy.” The scientific evidence suggests that some addicts do better with an emphasis on individual counseling, rather than the constant reliance on group work that traditional rehabs have to offer. As one counselor put it: “If I made an appointment to see a therapist because I was depressed, would I be told I have to do a program with everyone else?”
Monthly residential treatment can easily cost $25,000 or more. But public, government funded rehab centers, which presumably have less incentive to treat clients like money, are frequently full. And since these programs run the bulk of prison-related treatment in this country, addicts often stand a better chance of getting into these less expensive programs if they commit a crime.
Even if you manage to get in, rehab rules all too often seem arbitrary and punitive: Recreational reading materials, musical instruments, cell phones, and computers are frequently not permitted. And there is a strong tendency to insist that use equals abuse in every circumstance. Rehab management—the business of what happens after formal treatment ends—is largely neglected in the treatment sphere.
Fletcher rails against the disease model, but mostly in response to how she believes this concept is presented by AA/NA. Like other critics, she dwells on the idea that the disease tag serves as a crutch and an excuse, rather than as an extremely empowering notion for many addicts. In fact, the disease model, as addiction scientists understand it, is seriously underrepresented in the treatment field. Too many mental health professionals continue to insist that “all you need to do is get to the bottom of the problem and the need to use substances to cope, will dissipate,” said an M.D. specializing in addiction. “However, there is absolutely no evidence that this approach works for people who are addicted to alcohol or drugs… The primary-secondary issue is moot and an artifact of the bifurcation of the treatment delivery system.”
A significant number of rehabs still oppose medication-assisted treatment, Fletcher makes clear. Hazelden made news recently for dropping its long-standing opposition to buprenorphrine as a maintenance drug for opiate addicts during treatment. Richard Saitz of Boston University’s School of Medicine says in the book that if addiction were viewed like other health problems, “patients addicted to opioids who are not offered the opportunity to be on maintenance medications would sue their providers and win.”
According to Dr. Mark Willenbring, former director of the National Institute on Alcohol Abuse and Alcoholism (NIAAA): “No one wants to say, ‘Treatment as we’ve been doing it probably isn’t as effective as we thought, and we need more basic research to really come up with new tools. In the meantime let’s do what we can to help suffering people in the most cost effective way and strive to not harm them.’”
Monday, July 2, 2012
Supreme Court Decision: A Clear Win For Addiction Treatment?
A roundup of expert opinion.
Dr. Tom McLellan, chief executive officer of the Treatment Research Institute, who served on President Obama’s healthcare reform task force, called the recent U. S. Supreme Court Decision on the Affordable Care Act “the beginning of a new era in prevention, early intervention, and office based care for patients who are not addicted—but whose drinking, smoking, and use of other substances is harming their health and compromising the effectiveness of the care they are receiving for other illnesses and conditions.”
Mark Mishek, president and CEO of Hazelden, called the ruling “an essential step forward for millions of people who need help overcoming addiction… Expanding access to addiction treatment was a moral and financial imperative. It will save dollars, and, even more important, it will save lives.”
Phoenix House Chief Clinical Officer Dr. Deni Carise said the individual mandate “ensures that millions of Americans who struggle with addiction, but previously were unable to access or afford treatment, will now be able to receive the life-saving services they desperately need.” However, she worries about possible limitations in coverage: “It could be difficult to gain insurance coverage for non-hospital residential treatment, which is relatively unique to drug treatment.”
Now that the legality of ACA has been decided, we should work to implement it in a way that provides the treatment for addiction it was intended to provide,” said Mark Dunn, public policy consultant for the National Association of Addiction Treatment Providers (NAATP).
“This is a triumph for recovering Americans, many of whom were directly involved in advocating for the new law,” said Stanford psychiatry professor Keith Humphreys, another former White House adviser on drug policy. “Both the quantity and the quality of care for addiction are set for unprecedented—and long overdue—growth.”
Dr. David Shern, president and CEO of Mental Health America: “Of the estimated 32 million people who will gain coverage, about 4 to 6 million will have untreated mental illnesses or addictions. By including mental health and substance use services on the list of essential benefits… the law recognizes how integral behavioral health is to overall health. And it extends the groundbreaking Mental Health Parity and Addiction Equity Act and its prohibition of discriminatory limits on mental health and substance use services to those plans.”
Rahiel Tesfamariam, Washington Post: “We could start with what the new law will do for children struggling with mental illness and substance abuse, two challenges that often go hand-in-hand…. As a community organizer doing juvenile justice work in the Anacostia community of Washington, D.C. in recent years, I’d often come across children with behavioral issues rooted in untreated mental illness and substance abuse. It was heartbreaking to review case after case and find that proper medication and counseling could have prevented a lot of the young people we served from ever entering the criminal system. The systemic failure to meet their medical needs was a major contributing factor in the revolving door of delinquency and arrest that so many of them were trapped in.”
Aziz Huq is an assistant professor at the University of Chicago Law School: “There is, then, the possibility that some state states… will refuse the marginal increases in Medicaid funding that underwrite its expansion on ideological grounds…If states take this path, those not covered by the Medicaid expansion will continue to obtain healthcare in inefficient and expansive ways — undermining the cost-containment goals of the law and perhaps even threatening the stability of reduced premiums for others.”
Jeremy B. White, International Business Times: “But Republican governors are already renouncing the measure as a budget-buster. In a press release, [Florida Governor] Scott rejected spending ‘approximately $1.9 billion more taxpayer dollars required to implement a massive entitlement expansion of the Medicaid program.’ Scott also joined his Republican counterparts in refusing to implement the private health insurance exchanges that are the centerpiece of the law. Americans who earn under a certain amount but are not poor enough to qualify for Medicaid would get government subsidies to help them purchase insurance on the insurance exchanges, where different insurance companies would compete to appeal to customers.”
Photo Credit: http://www.urbanfaith.com
Thursday, June 14, 2012
Random Notes from the College on Problems of Drug Dependence
Opening day addresses at the annual meeting.
(These are notes on research in progress, not findings written in stone).
--NIDA director Nora Volkow talked up buspirone (Buspar) as a treatment for cocaine addiction, and referred to favorable results on buspirone for cocaine self-administration in monkeys in a large clinical trial. Also, different vaccine strategies are in the works, including different pharmacological approaches to blocking specific dopamine transporter molecules.
--Edward Sellers of DL Global Partners, a drug research consulting firm, emphasized the importance of enzyme variations in smoking. Variants of the CYP2A6 enzyme of metabolization allow us to identify “slow metabolizers” who respond well to placebo or nicotine patch therapy, and other smokers who don’t.
--Sherry McKee of the Yale University School of Medicine reminded everyone that cigarette smokers—even very light smoking “chippers”— are far more likely to have concurrent drinking problems than non-smokers. Smoking helps drinkers drink more and longer. To demonstrate such “potentiated reinforcement,” she showed a delightful video of her child eating cookies, then craving a glass of milk, then succumbing to another round of cookie consumption…
--Jack Henningfield of Pinney Associates, and former NIDA research chief, said that the reason the National Institute on Alcohol Abuse and Alcoholism (NIAAA) became an agency focused on “one molecule” is because Senator Harold Hughes, recovering alcoholic from Iowa, and Bill W., co-founder of Alcoholics Anonymous, wanted it that way.
--David Penetar of Harvard Medical School and McLean Hospital added more evidence of the link between alcohol and cigarettes, noting that “90 per cent of smokers drink,” and that smokers are three times as likely to be alcoholics than non-smokers. He pointed to research documenting a disturbing “increased desire to drink” when wearing a nicotine patch. With a patch, subjects reported feeling the effects of alcohol sooner and longer.
Photo Credit: http://www.thejournalshop.com/
Sunday, April 15, 2012
Ivan Oransky on the Disease Model at TEDMED 2012
What we think about when we think about “disease.”
It’s a safe bet that the number of M.D.s who have made a mid-career switch to journalism is rather small. And when Dr. Ivan Oransky did it, he didn’t go in for half measures. The former online editor of Scientific American, and the former deputy editor of The Scientist, Oransky now serves as Executive Editor of Reuters Health. He teaches medical journalism at New York University, where he also holds an appointment as clinical assistant professor of medicine—while maintaining three, yes three, separate blogs. He is well known for two innovative blogs known as Retraction Watch and Embargo Watch. And he recently kicked off a personal blog, the Oransky Journal.
So clearly, he’s a very lazy man. Nonetheless, he found time to give a very popular talk on the shortcomings of the disease model of medicine at last week’s TEDMED conference in Washington, D.C. And he found additional time to grant me an interview afterwards, with some interesting thoughts on how the mania for medicalization could affect addiction treatment.
Speaking at the Kennedy Center for the Performing Arts, Oransky compared patients in the nation’s current medical system to baseball coach Billy Beane, a once-promising player who washed out in the minors and was recently portrayed by Brad Pitt in the movie Moneyball. “Our medical system is just as bad at predicting what’s happening to patients as baseball scouts were at predicting what would happen to Billy Beane,” Oransky told the audience of 1,500.
“Every day, thousands of people across the country are diagnosed with pre-conditions,” he said. “We hear about pre-hypertension, we hear about pre-dementia and pre-anxiety. We also refer to sub-clinical conditions, like sub-clinical hardening of the arteries. One of my favorites is called sub-clinical acne. If you look up their website as I did, you’ll see that they say this is the easiest acne to treat. You don’t have any pustules or inflammation—you don’t actually have acne. I have a name for preconditions—I call them preposterous.”
Every year, according to Oransky, “we are spending more than two trillion dollars on health care," and yet more than 100,000 people a year are dying from complications of the treatments they're getting, rather than from the conditions that are being treated. [Revised 4-15]. And most patient advocacy groups eventually learn to “expand the number of people who are eligible for a given treatment” for fundraising purposes, he said.
As evidence of this trend toward medicalization, Oransky pointed to the novel notion of a “previvor.” According to FORCE, the cancer research advocacy group that coined the term: "A previvor is a survivor of a predisposition to cancer.” The term is used to describe someone who, for example, has a genetic risk for breast cancer, but has not been diagnosed with the disease. “Previvor was coined in 2000 after a challenge from a community member who said she ‘needed a label,’” according to the group’s web site.
We are all previvors of some disorder, Oransky argues. In the spirit of giving everyone a precondition, Oransky coined the term “pre-death.” What is pre-death? “Every single one of you has it,” Oransky told the audience, “because you have the risk factor for it, which is being alive."
Using his favorite metaphor—baseball—Oransky explained the secret of Billy Beane’s revolutionary success as a coach: “The secret wasn’t to swing at every pitch, like the sluggers do. You had to find the guys who liked to walk, because getting on base by a walk is just as good. And in our health care system, we need to figure out, ‘is that really a good pitch, or do we need to let it go by, and not swing at everything?’ We all need to keep in mind that in medicine, sometimes less is more.”
After his talk, I asked Oransky how the theme of medicalization might apply to the disease of addiction. Medicalization, he said, is a matter of “taking advantage of people, manipulating them so they can’t make informed decisions.” In the case of addiction treatment, Oransky pointed to the “proliferation of ads for treatment in beautiful places. It’s all selling and self-diagnosis. They’re selling you on the fact that you need to be treated.” He also pointedly referred to the practice of “medical astro-turfing,” where a supposedly grass roots effort by patients or advocates is “usurped by interest group pressure.” Sometimes that usurpation is patently obvious, is in the case of many advocacy groups set in motion and funded by pharmaceutical companies or the liquor industry.
Sometimes, of course, you do need to be treated. And Oransky notes that in health areas such as addiction and mental illness—disorders where social stigma remains high, compared to, say, a blood infection—there are “fewer pressures to medicalize.” And possibly, too few pressures to medicalize. “There’s no quick and easy test, no MRI where you can point to the place in the brain that lights up and say, “you are an alcoholic.” The science of addiction, which has been moving by fits and starts into the medical mainstream, has a long way to go, compared with many other disease categories. And it has left a gap through which medical workers and treatment staff can march, chanting, “I have a system,” Oransky says.
Perhaps, then, the study of addiction to alcohol and other drugs requires both more medicalization of the research kind, and less of the “precondition” or “sub-clinical” kind. As for the second kind, Oransky believes we are already medicalizing binge drinking in a counterproductive way. In addition, “there are always attempts to widen the market. Look at how obesity has been made to overlap with addiction.” As for medications being used to combat craving among addicts in treatment, Oransky noted the tendency to “repurpose” drugs on the basis of soft data. “They took wellbutrin, an antidepressant that didn’t work very well, and offered it for smoking cessation. So I would want to see data that is really robust” before treating addicts with such medications.
On the other hand, Oransky noted, “We don’t have to worry about malaria, we don’t need to medicalize tuberculosis. But do diseases that have a strong stigma, like addiction, actually benefit from medicalization? If we find out that they do, than we should do it.”
There’s something else Oransky believes is overdue for true medicalization: “The social determinants of health care—poverty, the way we build our suburban environments. Concentrate on stuff that we know kills people. Medicalize that.”
In the end, he said, “we need to use marketing strategies to effectively get treatment to the people who need it, not to the people who don’t.”
Tuesday, March 13, 2012
Interview with Deni Carise, Chief Clinical Officer of Phoenix House
Why addiction treatment works—if you let it.
This time around, our “Five-Question Interview” series features clinical psychologist Deni Carise, senior vice president and chief clinical officer at Phoenix House, a leading non-profit drug treatment organization with more than 100 programs in 10 states. Chances are, you may have seen or heard her already: Dr. Carise has been a guest commentator about drugs and addiction for Nightline, ABC’s Good Morning America, Fox News, and local New York media outlets. She is frequently quoted in US News and World Report and other periodicals, blogs at Huffington Post, and has also consulted for the U.N. Office on Drugs and Crime.
Dr. Carise earned her doctorate at Drexel University, and served as a post-doctoral fellow at the Center for Studies of Addiction at the University of Pennsylvania. Currently, she is also adjunct clinical professor in the University of Pennsylvania’s Department of Psychiatry. She has been involved with drug abuse treatment and research for more than 25 years, and has worked extensively in developing countries to integrate science-based drug treatments into local programs. She has worked with adults and adolescent populations including dually diagnosed clients, Native Americans, and with medical populations (including spinal cord-injured, cardiac care and trauma patients).
1. As chief clinical officer for Phoenix House Foundation, what's your job description?
Deni Carise: My main responsibility is to ensure that we provide the highest possible standard of care. This means making sure that treatment methods across our programs are consistent with the latest research, represent a variety of evidence-based practices, and are delivered with fidelity. I also collaborate on the implementation and evaluation of Phoenix House’s national and regional strategies to achieve clinical excellence. My home base is New York, but I work directly with all of our programs and regularly travel to our California, New England, Mid-Atlantic, Texas, and Florida regions. I also oversee the activities of our Family Services, Quality Assurance, Research, Workforce Development, and Training initiatives. Finally, I help Phoenix House spread awareness to the public about the need to reduce the stigma of addiction and to increase access to treatment services.
2. As a clinical psychologist, how did you become involved in drug and alcohol treatment and recovery?
Deni Carise: I actually became involved in the Substance Abuse Treatment (SAT) field prior to becoming a clinical psychologist. When I decided that I wanted to get sober, I got some help from a counselor. This counselor was so helpful to my recovery that I decided to become an SA counselor so that I could assist others on this journey. I was working as a model at that time, and there were a few aspects of that career that I didn’t like: First, it was very clear that I would become less valuable in my career as I got older; secondly, my value was exclusively based on appearance, not knowledge or skills; and finally, my work didn’t contribute to the greater good—that is, no one benefitted by my work. I wanted a new career where I would become more valuable as I got older and more experienced, and where my knowledge and skills would be of value. I also wanted to do something I felt was contributing to society. The SAT field seemed to fit all these criteria.
3. What makes it so difficult for people to accept the disease components of serious drug addiction?
Deni Carise: People have difficulty accepting the disease concept of addiction for three reasons. First, people believe addiction is self-induced; you wouldn’t have it if you didn’t use drugs, right? There is some truth to this, but of all those who try drugs, an estimated 5 to 10% (depending on the drug) will become addicted. There’s a reason why the other 90 to 95% don’t become addicted.
That brings us to reason #2: People generally don’t believe there is a genetic cause. It is now very clear that there is a genetic component to substance use disorders. For example, if a father is an insulin-dependent diabetic, the heritability estimates range from 70 to 90% likelihood that the man’s son will also be diabetic. For hypertension, the heritability estimates are from 25 to 50%, depending which study we look at. For alcohol, the estimates are 55 to 65% likelihood that a young man will be alcohol dependent if his father is. For opiate dependence, it’s 35 to 50%.
The third and probably most important reason is that people think calling addiction a disease absolves the substance abuser of responsibility for his or her actions. Nothing could be further from the truth. Those in recovery see the disease of alcoholism or addiction as a moral obligation to get well. If you know you have this disease and the only way to keep it under control is not to use alcohol or drugs, then that’s what you have to do.
4. Overall, treatment doesn't seem to be that effective. What's missing?
Deni Carise: I believe treatment is effective. We’re just expecting the wrong results. Substance abuse has the same characteristics as any chronic medical disorder. The problem is that we (society, families, even me) want addiction to respond to treatment as though it’s an acute medical problem, like a broken leg or appendicitis. If it were an acute problem, we could send our kids, loved ones, even ourselves to treatment for a set number of days (maybe 7, maybe 28) and leave the hospital or treatment facility with the condition cured—as we would after surgery for an appendicitis! I would love that.
Unfortunately, we’ve been measuring treatment success the same way we would for a surgical problem, even though substance abuse and dependence are, in fact, chronic problems. Think about this—substance abuse treatment success is often measured by symptoms, drug use, and life problems prior to treatment and again six months after treatment ends. Imagine if we measured success of diabetes treatment the same way. We would measure their blood sugar levels, weight, number of diabetic crises, and other related problems before treatment. Then we’d send them off to a treatment program where we would prescribe medications, maybe give them insulin, teach them about a good diet, discharge them (take away that treatment), and measure their blood sugar levels, weight, etc. six months after we stopped the medication. Do we really think that would work with diabetes? Then why would we think it would work with addiction?
As with all chronic disorders, there are no prolonged, symptom-free periods without continued attention and self-management of the illness. Just as some people with diabetes can manage their illness with behavioral changes such as making healthy decisions when offered cakes or cookies, or starting an exercise program, some people with substance abuse problems can control their symptoms by changing their behaviors. This means not being around others who use, making the right decisions when offered alcohol or drugs, etc. For those who can’t do this alone, there’s treatment to teach them how to manage their disease and there are medications to assist them. And I’m talking about the diabetic and the substance abuser.
So treatment can work, but, just like any chronic disease, there’s no quick fix.
5. You're committed to working with developing countries to bring scientifically valid treatment within reach of poorer populations. How is the effort going?
Deni Carise: I’ve been really lucky to be able to consult for numerous treatment systems, universities, and countries around the world—including training clinicians from Nigeria, Thailand, Egypt, Greece, Iran, Singapore, Brazil, China, Iraq, India, and other countries. It’s fascinating to see how different countries approach local substance abuse problems. Some countries have historically asserted that substance abuse is not a problem in their communities, so for them to offer treatment of any kind means they need to change their socipolitical stance. That doesn’t happen quickly. For one country, the diagnosis of AIDS among 7 substance abusers who had shared needles was the impetus to providing treatment.
Much of what I’ve done internationally involves cultural adaptations of standardized instruments or clinical tools (such as the Addiction Severity Index assessment tool) for use within various cultures. To do this, I typically meet with numerous staff who deliver direct services in the country. We go over each assessment question or worksheet item looking at what would make sense in their culture. Types of things that frequently need adapting are questions about education (not everyone has “high schools”), employment and income, demographic questions such as race categories, and all manner of expressions used to describe drugs and clinical symptoms. Then we pilot the new interview or service with some local clients and get their perspective and make a final version.
Much of this work has been funded by the United Nations Office on Drug Use and Crime, the National Institute on Drug Abuse and Office of National Drug Control Policy.
Subscribe to:
Posts (Atom)